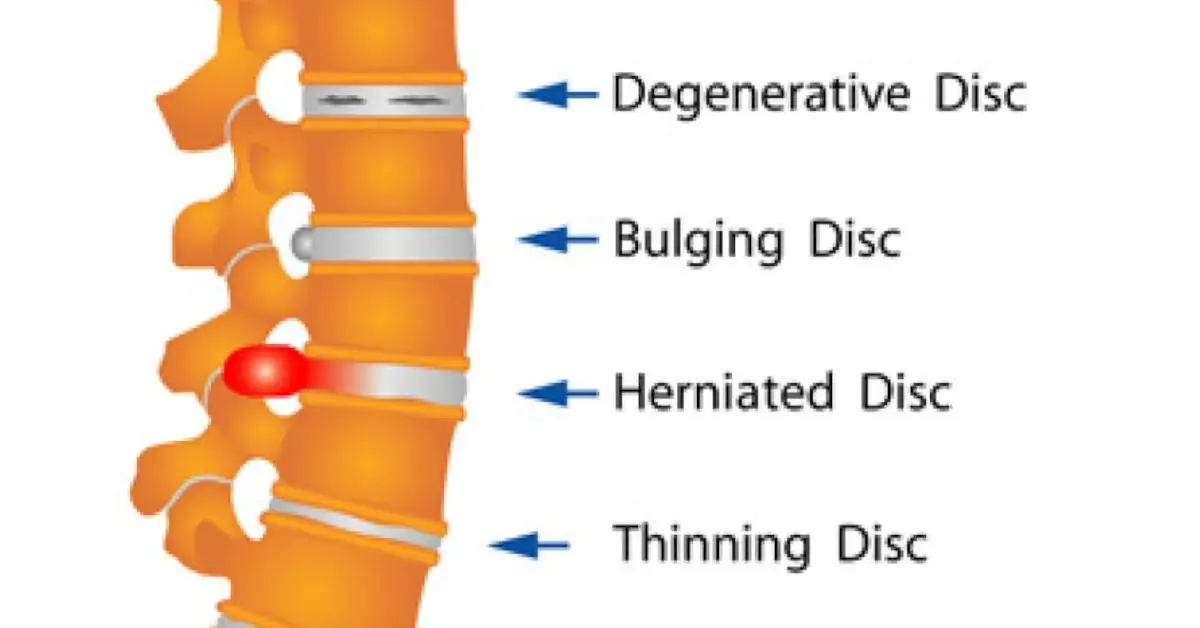
Discogenic back pain, or lumbar disc pain, is the result of degeneration of lumbar intervertebral discs in the lower back. This degeneration is a normal part of the aging process, and it is unknown as to why certain degenerative disks cause so much pain. Of the patients with chronic lower back pain, 26%-42% suffer from this ailment. Those most commonly affected are between 30 and 60 years old. Once a disc has fully degenerated, it no longer has inflammatory proteins that can cause pain and enters into a stable position. This is why discogenic pain rarely occurs after 60 years of age.
An estimated 6 million people in the U.S. live with chronic discogenic pain, yet relief is possible with proper medical attention.
When diagnosing discogenic back pain, doctors look at the patient’s medical history, analyze the presenting symptoms, and perform a physical exam to assess the problem. In some cases, a CAT scan or MRI may be useful if the physical assessment does not yield clear results, or if a patient is not responding to treatment.
Those affected by discogenic back pain can experience varying levels of pain. The pain can happen during physical activity or even when there is no exertion. Pain can worsen during sneezing or coughing, which both increase the pressure between discs. Areas that experience pain along with the lower back include the buttocks, groin, or thighs.
In some cases associated tingling or numbness can be felt all the way in the foot, making attempts to walk difficult. Patients can feel like it is difficult to fully straighten their backs and may also find it difficult to remain seated for extended periods of time. Symptoms are often most relieved by a fully reclined position.
Once a patient has been diagnosed with discogenic back pain, there are a number of treatment options available to him or her, depending on the severity of the pain and presentation of symptoms. One of the first defenses is strict bed rest, especially in severe cases. Spending extended hours in bed can help to relieve pressure on the disturbed disc. In order for the disc to heal, however, the patient must allow it to bear some weight, which precludes bed rest as a permanent solution.
Physical therapy can be a helpful tool in treating and managing the pain through exercises that strengthen back muscles and can be maintained at home. If back muscles become stronger and more flexible, weight is distributed more evenly and there is less pressure on the disc. Anti-inflammatory medication can be prescribed by a doctor or purchased over the counter and is helpful in lowering the pain to tolerable levels. Sleep medication may also be prescribed to patients dealing discomfort that leads to difficulty sleeping. Surgery can/may be required in more severe cases.
The only known ways of possibly preventing this kind of back pain are by exercising, not smoking, and avoiding lifting heavy loads. A healthy lifestyle is always the best preventative medicine for back pain, but is not always a guarantee.
Dr. Steven Horowitz evaluates patients and determines what the best path of treatment will be based on their presenting symptoms and pain level. Specializing in pain management, he understands the most effective ways of making patients have optimal comfort and feel their best at all times. Chronic back pain can prevent you from living a full, active life. Dr. Horowitz ensures that by managing pain you can return to living the life you want to.